Contents
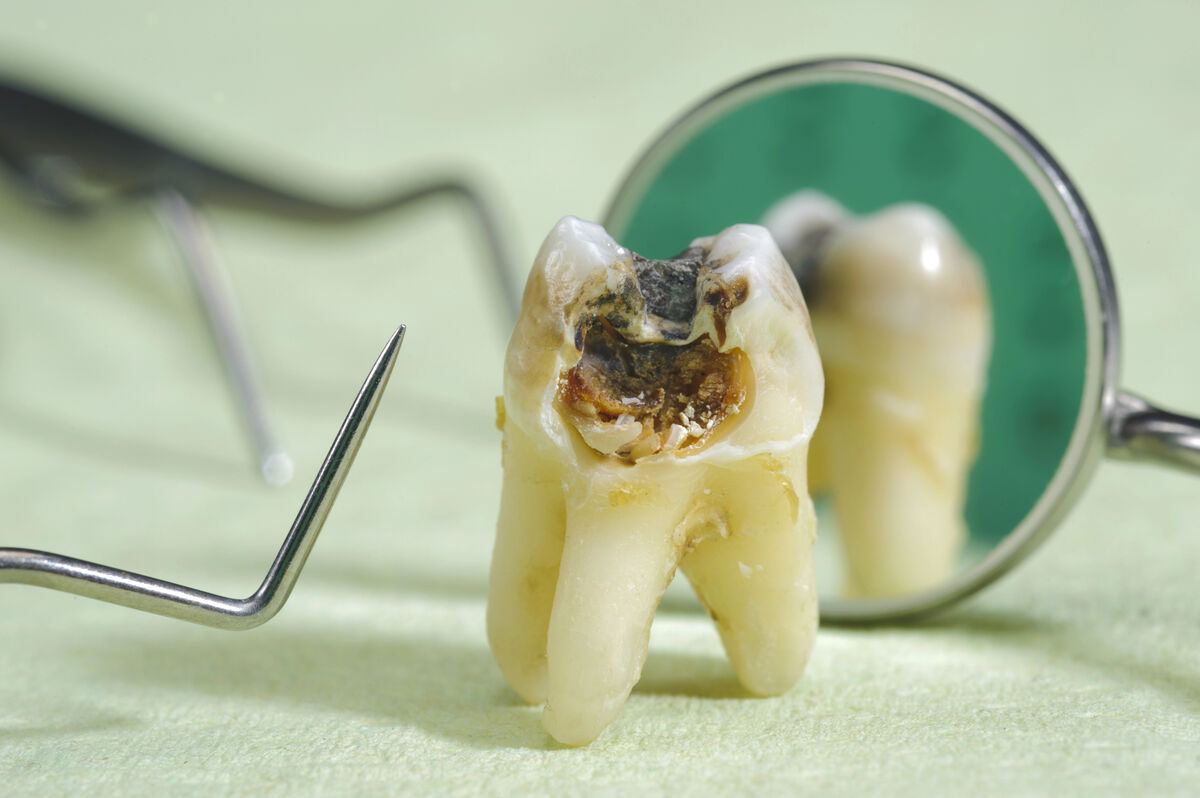
Dental Cavities in 2026: Causes, Symptoms, Treatments, and Prevention Guide
Dental cavities remain the single most common chronic disease worldwide, affecting an estimated 2.3 billion people according to the World Health Organization. In the United States alone, the CDC reports that over 90% of adults have had at least one cavity, and roughly 26% of adults currently have untreated tooth decay. Despite being almost entirely preventable, cavities continue to cause pain, tooth loss, and billions of dollars in treatment costs every year.
The good news is that advances in diagnostic technology and restorative materials mean that catching and treating cavities in 2026 is more effective, more comfortable, and more durable than ever before. This guide walks you through everything from the biology of how cavities form to the latest treatment options and their costs, so you can take control of your oral health with confidence.
Good to Know: A dental cavity (also called dental caries or tooth decay) is a permanently damaged area in the hard surface of a tooth that develops into a tiny opening or hole. Left untreated, it grows larger and can eventually destroy the tooth entirely.
What Is a Dental Cavity and How Does It Form
A cavity is the result of a process called demineralization. Hundreds of species of bacteria naturally live in your mouth, forming a sticky film called dental plaque. When you eat or drink foods containing sugars or starches, certain bacteria in the plaque -- particularly Streptococcus mutans and Lactobacillus -- metabolize those sugars and produce acids as a byproduct.
These acids attack the mineral structure of your tooth enamel, dissolving calcium and phosphate ions in a process called demineralization. Your saliva naturally works to counteract this by supplying minerals back to the enamel (remineralization) and buffering the acids. However, when the rate of demineralization consistently outpaces remineralization -- due to frequent sugar exposure, poor hygiene, or insufficient saliva flow -- the enamel weakens and eventually breaks down, forming a cavity.
Once the cavity penetrates through the enamel into the softer dentin layer beneath, the decay accelerates. If it continues unchecked, bacteria reach the dental pulp (the nerve and blood supply inside the tooth), causing pulpitis -- the throbbing toothache many people associate with cavities.
"Cavities are not inevitable. They are a bacterial infection driven by diet and hygiene. When we reframe cavities as a preventable disease rather than a dental inevitability, patients become more empowered to take action."
Primary Causes and Risk Factors for Tooth Decay
Cavity formation is multifactorial. Understanding the interplay of these risk factors is essential for effective prevention.
Dietary Factors
- Frequent Sugar Consumption: Every time you eat or drink something sugary, your mouth pH drops for about 20 to 30 minutes. Frequent snacking or sipping sugary drinks throughout the day keeps the pH low, giving acid more time to attack enamel.
- Sticky and Starchy Foods: Caramels, dried fruit, crackers, and chips cling to tooth surfaces longer, providing prolonged fuel for bacteria.
- Acidic Beverages: Sodas, sports drinks, citrus juices, and even sparkling water with citric acid directly erode enamel, making it more vulnerable to bacterial acid.
Oral Hygiene Habits
- Inadequate Brushing: Brushing less than twice a day or using improper technique allows plaque to accumulate in crevices and along the gumline.
- Skipping Floss: Toothbrush bristles cannot reach the tight contact areas between teeth. Without flossing or using interdental brushes, these surfaces become prime sites for interproximal cavities.
Biological and Medical Factors
- Dry Mouth (Xerostomia): More than 500 commonly prescribed medications -- including antihistamines, antidepressants, and blood pressure drugs -- reduce saliva flow. Without adequate saliva, the mouth loses its primary defense against acid.
- Enamel Defects: Conditions like enamel hypoplasia or amelogenesis imperfecta create thin or porous enamel that is highly susceptible to decay.
- Deep Tooth Anatomy: Molars with deep pits and fissures trap food and bacteria more readily than smooth-surfaced teeth.
- Genetics: Research suggests that genetic factors influence enamel thickness, saliva composition, and immune response to oral bacteria.
The Five Stages of Cavity Progression
Cavities do not appear overnight. They progress through distinct stages, and treatment depends on how far the decay has advanced.
| Stage | What Is Happening | Symptoms | Reversible? |
|---|---|---|---|
| 1. Initial Demineralization | White or brown spots appear on enamel surface | Usually none | Yes, with fluoride and hygiene |
| 2. Enamel Decay | Enamel breaks down; small cavity forms | Mild sensitivity to sweets | No -- requires a filling |
| 3. Dentin Decay | Decay reaches softer dentin layer | Sensitivity to hot, cold, sweets | No -- filling or onlay needed |
| 4. Pulp Involvement | Bacteria reach the nerve (pulpitis) | Severe, throbbing, spontaneous pain | No -- root canal needed |
| 5. Abscess Formation | Infection spreads beyond tooth root | Swelling, fever, pus, intense pain | No -- root canal or extraction |
Warning: A cavity can reach the dentin stage without causing any noticeable symptoms. By the time you feel pain, the decay is often advanced. This is why twice-yearly dental check-ups with X-rays are critical for early detection.
Recognizing Cavity Symptoms at Every Stage
Early cavities are silent. As the decay progresses, you may notice:
- White, brown, or black spots on a tooth surface
- Sensitivity when eating or drinking something sweet, hot, or cold
- A visible hole or pit in the tooth
- Pain when biting down
- Spontaneous toothache that wakes you at night
- Persistent bad breath or a foul taste
- Swelling of the gum near the affected tooth
If you experience any of these symptoms, schedule a dental appointment promptly. The earlier a cavity is diagnosed, the simpler, less invasive, and less expensive the treatment will be.
How Dentists Diagnose Cavities in 2026
Modern dentistry employs several tools to detect cavities, often before they are visible to the naked eye:
- Visual and Tactile Examination: Using a dental mirror and explorer to inspect each surface for discoloration, soft spots, or roughness.
- Digital X-rays: Bitewing radiographs reveal decay between teeth and under existing restorations. Digital sensors use up to 80% less radiation than traditional film.
- Laser Fluorescence Detection: Devices like DIAGNOdent use laser light to detect early demineralization in enamel before a cavity has formed, enabling truly preventive intervention.
- Intraoral Cameras: High-resolution cameras capture magnified images of each tooth, helping both the dentist and the patient see areas of concern.
"With laser fluorescence and AI-assisted radiographic analysis, we are catching cavities at the white-spot stage -- before they become actual holes. This shift toward early detection is transforming preventive dentistry."
Modern Cavity Treatments and Their Costs
Treatment depends on the stage of the cavity. Here are the current options and their estimated costs in 2026:
| Treatment | When It Is Used | Estimated Cost (2026) |
|---|---|---|
| Fluoride Treatment / Silver Diamine Fluoride | Stage 1 (initial demineralization) | $30 - $75 per application |
| Composite Resin Filling | Stages 2-3 (enamel/dentin decay) | $175 - $400 per tooth |
| Ceramic Inlay or Onlay | Large Stage 3 cavities | $800 - $1,800 per tooth |
| Dental Crown | Extensive decay, post-root canal | $1,000 - $2,500 per tooth |
| Root Canal + Crown | Stage 4 (pulp involvement) | $1,500 - $3,500 total |
| Extraction + Replacement | Stage 5 (tooth unsalvageable) | $200 - $600 (extraction only) |
Dental insurance typically covers preventive fluoride treatments at 100%, basic fillings at 70-80%, and major procedures (crowns, root canals) at 50%. Coverage depends on your specific plan, deductible, and annual maximum. Always request a pre-treatment estimate to avoid surprises.
Good to Know: Silver Diamine Fluoride (SDF) is a topical liquid that can arrest early cavities without drilling. It is painless, fast, and inexpensive -- making it especially useful for young children, elderly patients, and those with dental anxiety. The trade-off is that it stains the decayed area black, so it is typically used on non-visible surfaces.
Complications of Untreated Cavities
Ignoring a cavity does not make it go away -- it makes everything worse. Potential complications include:
- Dental Abscess: A pocket of pus forms at the root tip, causing severe pain, swelling, and fever. An abscess is a medical emergency that requires immediate treatment.
- Tooth Loss: Extensive decay may make the tooth unsalvageable, requiring extraction and subsequent replacement with an implant or bridge.
- Spread of Infection: In rare but serious cases, an untreated dental infection can spread to the jawbone, sinuses, or even the bloodstream (sepsis).
- Nutritional Problems: Pain while chewing leads people to avoid certain foods, potentially resulting in nutritional deficiencies.
- Impact on Quality of Life: Chronic dental pain affects sleep, concentration, work productivity, and mental health.
Warning: If you experience facial swelling, fever, difficulty swallowing, or pus draining from a tooth, seek emergency dental care immediately. These are signs of a spreading infection that can become life-threatening without prompt treatment.
Proven Prevention Strategies for 2026
Preventing cavities is far simpler, less painful, and less expensive than treating them. Here are the most effective strategies supported by current evidence:
- Brush Twice Daily with Fluoride Toothpaste: The ADA recommends brushing for two full minutes each time, using a soft-bristled brush and toothpaste containing at least 1,000 ppm fluoride.
- Floss or Use Interdental Cleaners Daily: Cleaning between teeth removes the plaque that brushing alone misses.
- Limit Sugary and Acidic Foods Between Meals: Confine sweets and acidic drinks to mealtimes when saliva flow is highest, and rinse with water afterward.
- Drink Fluoridated Water: Community water fluoridation reduces cavity rates by approximately 25%, according to the CDC.
- Chew Sugar-Free Gum with Xylitol: Xylitol inhibits the growth of cavity-causing bacteria and stimulates saliva production.
- Get Professional Cleanings Twice a Year: Regular prophylaxis removes tartar and allows your dentist to catch problems early.
- Consider Dental Sealants: Thin plastic coatings applied to the chewing surfaces of back teeth can reduce cavity risk by up to 80% in children and adolescents.
Cavities in Children: What Parents Need to Know
Tooth decay is the most common chronic childhood disease in the United States -- five times more common than asthma. Early childhood caries (formerly called "baby bottle tooth decay") can begin as soon as the first tooth appears.
Parents should start cleaning an infant's gums with a damp cloth after feedings and begin using a rice-grain-sized smear of fluoride toothpaste as soon as the first tooth erupts. The ADA and the American Academy of Pediatric Dentistry both recommend a child's first dental visit by age one or within six months of the first tooth appearing.
Key prevention tips for children include avoiding putting sugary liquids in bottles, not sharing utensils (which transfers cavity-causing bacteria), and applying dental sealants as soon as permanent molars come in (typically around ages 6 and 12).
"We now know that cavity-causing bacteria can be transmitted from caregiver to child through saliva. Simple steps like not sharing spoons and establishing brushing routines early can dramatically reduce a child's cavity risk."
Frequently Asked Questions
Can a cavity heal on its own?
Only at the very earliest stage. When demineralization has created a white spot but has not yet broken through the enamel surface, aggressive fluoride therapy, improved hygiene, and dietary changes can reverse the process. Once an actual hole has formed in the enamel, the damage is permanent and requires professional treatment.
How much does it cost to fill a cavity in 2026?
A composite resin filling -- the standard tooth-colored option -- typically costs between $175 and $400 per tooth without insurance. With a dental plan that covers basic restorative at 70-80%, your out-of-pocket cost may be as low as $35 to $120 per filling after your deductible is met.
Are silver amalgam fillings still safe?
According to the ADA and the FDA, dental amalgam remains a safe and effective filling material for most patients. However, the FDA updated its guidance in 2020 to recommend that certain groups -- including pregnant women, nursing mothers, children under six, and people with kidney disease -- consider alternatives when possible. Many patients and dentists now prefer composite resin fillings for both aesthetic and precautionary reasons.
How often should I see a dentist to catch cavities early?
The standard recommendation is every six months for most adults. However, patients with a higher risk of cavities (history of frequent decay, dry mouth, diabetes, active orthodontic treatment) may benefit from visits every three to four months. Your dentist can help determine the ideal schedule based on your individual risk profile.
Can you get a cavity under an existing filling or crown?
Yes. This is called recurrent or secondary caries. Bacteria can seep through micro-gaps between the filling and the tooth, especially as older fillings wear or chip. Regular dental X-rays are essential for detecting this type of hidden decay before it causes significant damage.
Sources
- World Health Organization. "Oral Health Fact Sheet." WHO Global Oral Health Programme, 2024.
- Centers for Disease Control and Prevention. "Oral Health Surveillance Report: Trends in Dental Caries." CDC NCHS Data Brief, 2025.
- Featherstone JDB. "The Caries Balance: The Basis for Caries Management by Risk Assessment." Oral Health and Preventive Dentistry, 2024;22(1):15-28.
- American Dental Association. "Fluoride: Topical and Systemic Supplements." ADA Clinical Practice Guidelines, 2025.
- Fontana M, et al. "Early Detection of Caries Lesions Using Laser Fluorescence." Journal of Dental Research, 2024;103(4):389-397.
- FDA. "Dental Amalgam Fillings: Recommendations for Certain High-Risk Groups." FDA Safety Communication, 2020 (reaffirmed 2024).
- American Academy of Pediatric Dentistry. "Policy on Early Childhood Caries." Reference Manual, 2025.
- National Institute of Dental and Craniofacial Research. "Dental Caries in Adults (Age 20-64)." NIDCR Data Tables, 2025.
